IDJWI ISLAND — From my home in Idjwi, an island in Lake Kivu between the Democratic Republic of Congo and Rwanda with a population of 300,000, I’ve been watching the U.S. measles outbreak with a mixture of astonishment and incredulity.
The U.S. outbreak, with nearly 1,000 reported cases so far, is due in large part due to parents who have not vaccinated their children against this highly contagious disease. In Idjwi, many parents would give anything for their children to receive a measles vaccination, because they know all too well what can happen to unvaccinated children.
My wife and I run Amani Global Works, a nonprofit organization designed to serve as a bridge from the fractured medical care available in Idjwi to a modern health care system, and also to build defenses against epidemics through integrated primary care. Despite the island’s relatively small population, we have seen more than 1,500 cases of measles at our hospital. The real figure is surely much higher, since most people can’t access the hospital. The known death toll is 100, and rising.
Vaccination is currently the surest means of preventing measles. But in Idjwi it is quite difficult for individuals to receive the vaccine. One reason is that the Democratic Republic of Congo has more than 500 health zones, and Idjwi is one of the last to be supplied with vaccines — and that happens only after an epidemic has been confirmed and declared, usually after many have died.
Almost all of Idjwi’s 83 villages are last-mile communities, far removed from modern medicine. With just 22 ill-equipped health posts to cover an island five times the size of Manhattan, Idjwi has only 11 doctors and 100 nurses for its 300,000 inhabitants. This makes it close to impossible to fight any epidemics without relying on a cadre of professional, trained, paid, and supervised community health workers. Integrating such a cadre into the island’s nascent health system has been a challenge, but it is the only way to address health issues, carry out preventive campaigns, and address epidemics effectively and efficiently.
Similar issues have dogged the Democratic Republic of Congo’s response to its latest Ebola outbreak, which has killed more than 1,000 people since erupting last August in a region about 400 kilometers north of us.
But while Ebola has grabbed the headlines, the primary concern in Idjwi is measles. One family lost three of its children to measles in one week. Some parents bring their children to the hospital too late, and the nurses or community health workers are unable to do anything. Instead, they ask parents and staff to pray and wait for the child to die.
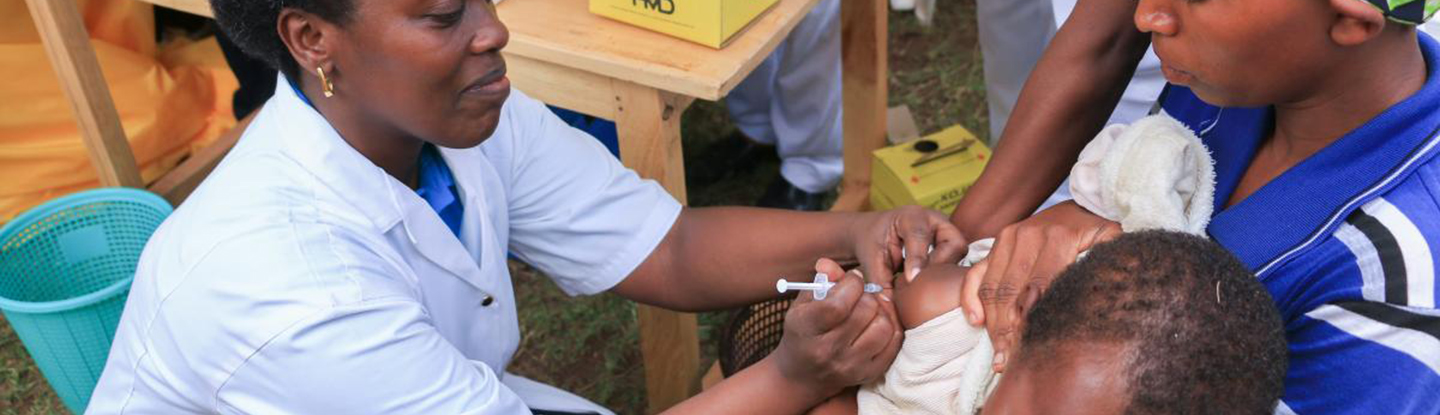
Children being vaccinated at an Amani Global Works hospital in Idjwi.COURTESY JACQUES SEBISAHO
“Measles is worse than malnutrition, pneumonia, and diarrhea combined,” said Tuombe Kabidu Victor, a nurse at the Idjwi Island hospital, holding a child who just recovered from the measles.
The child, a 2-year-old named Glodi, is lucky. Although his mother had been unable to procure a vaccination for him, she was able to reach the hospital in time when she observed spots on his body. Many children in other villages haven’t been so lucky. In one village, we learned about 10 children dying from measles in one week.
People here understand that vaccinations can mean the difference between life and death for their children. Many actively put pressure on their local leaders to provide vaccines for them. While some people in the United States and other countries are writing or advocating that vaccines are harmful, and are pumping resources into such campaigns, the residents of Idjwi are beseeching leaders to vaccinate its 300,000 souls.
“We have buried many children in our village who would never have died if they had a chance to get measles vaccine!” says Rehema, young Glodi’s mother.
Vaccines are a source of hope for a community that has suffered from thousands of avoidable deaths, or “mort bête,” as Paul Farmer, the founder of Partners in Health, describes them. To ensure more people can get vaccinated, Amani Global Works is building a replicable unit of primary health care delivery: community health workers delivering care in the home, nurses and midwives providing care in functional health centers, and referral hospitals (Idjwi technically has four hospitals, but only two truly fulfill the criteria of a hospital) handling complicated cases. This system reaches all residents at the three important public health locations: the community, the health clinic, and the hospital. It also solves geography and distance challenges during mass drug or vaccination campaign because community health workers, who live in their respective communities, and are first-line responders who bring vaccines and other appropriate drugs to the home. We are currently using this model in the northern part of the island, and plan to do the same in south Idjwi by 2022.
If parents in Idjwi were given the chance offered to their American counterparts to easily vaccinate their children, they wouldn’t miss the opportunity for anything in the world. Parents in the U.S. shouldn’t, either.